Encephalitis
Encephalitis is an inflammation of the brain tissue, the brain mass. This causes direct damage to nerve cells or the white matter of the brain.
It is important to know that it does not happen that two people have the same encephalitis, nor do they have all the complaints listed. Depending on which brain area is most affected, complaints may also differ. Early and adequate diagnosis and treatment give a better prognosis.
Symptoms of encephalitis may be initially mild, but may become more severe over the course of hours or days.
Early and adequate diagnosis and treatment offer a better prognosis.
Parental intuition may be life-saving.
Quote:
Regarding babies: if you, as a parent, don't trust your child's illness, go to the GP or emergency clinic. Your intuition is rarely wrong.
I started "peddling" my sick baby at night. As a result, he was already in the hospital when the illness really broke out. That saved his life.

Complaints of encephalitis
The disease usually starts with a high fever and flu symptoms. Within one to a few days, the patient develops serious complaints such as epileptic seizures, loss of consciousness, half-sided paralysis, vision problems and aphasia.
This leads to rapid referral from the GP to the emergency room. If the disease is treated, it can take weeks and in some cases months before someone can leave the hospital.
Brain damage often occurs, such as problems with thinking, weakness of the limbs and walking disorders, so that the patient must first be rehabilitated. The subsequent recovery often takes months.
The complaints may be:
- high fever
- flu-like symptoms (headache, fever)
- severe headache
- hypersensitivity to light
- other forms of overstimulation for sound, smell or movement
- nausea and vomiting
- loss of consciousness / coma
- (muscle) weakness
- eye muscle paralysis
- problems with vision/double vision
- epilepsy / seizures
- half-sided paralysis
- aphasia / difficulty speaking
- memory problems
- Neck stiffness/neck pain or back stiffness, neck spasm (in the mixed form with meningitis), which, in babies or very young children, may cause the child to cry when changing diaper or when bringing the head forward with the chin to the chest. This is due to increased sensitivity or pain, as tension is placed on the spinal cord and meninges. Children with meningitis hold their heads back very tensely.
Note: In babies, a stiff neck is often not present, even with confirmed meningitis. In children over one year old, a stiff neck is a better indicator of meningitis than in younger children.
Summarized:
- Brudzinski's sign (automatic leg lifting when the head is bent forward)
- Kernig's sign (severe pain when extending a bent knee)
- Diaper pain during diaper changes
- drowsiness/apathy
- loss of appetite
- intestinal complaints
- confusion / acute confused behavior (in that case rest and restriction of visitors are necessary!)
- Memory problems
- Coordination problems
- Agitation
- Hallucinations, hearing and seeing things that aren't there
- Rash (small red spots, blisters, or even a more extensive rash) A rash can occur as a result of an underlying infection, such as a virus that causes encephalitis
When the brain swells due to inflammation
The brain is protected in the hard shell, the skull. When the brain starts to swell, the skull holds back the swelling, causing the swollen brain to look for a different direction.
This may cause them to put pressure on the brain stem.
This part of the brain regulates vital functions such as breathing and heart rate.
When this situation is left untreated, cerebral pressure increases
and the brain stem may stop functioning and the patient will die.
Types of encephalitis by cause / drop-down menu
Meningoencephalitis, the mixed form
The distinction between meningitis and meningitis is blurred, because encephalitis often also involves inflammation of the meninges. This mixed form is called meningoencephalitis.
Long-term consequences of encephalitis
The consequences depend on which part of the brain the infection was occurred. See our page about complaints and consequences per brain area.
Moreover, functions are often spread over several brain areas.
The age at which one becomes ill also has an influence, as does the severity of the infection.
Some forms are very mild and some are much more serious. A multitude of different complaints are mentioned.
Someone can be left with residual symptoms from these serious infections, such as:
- epilepsy due to scar tissue
- spasticity
- fatigue
- changed sleep pattern
- malaise
- memory problems
- changed eating pattern
- overstimulation: sensory processing disorder (it is important to provide a low-stimulus living environment)
- irritability and apathy (also called postencephalitic syndrome)
- changes in sexual behavior
- behavior of putting objects in the mouth
Post-encephalitic syndrome
Post-encephalitic syndrome means that after a brain infection a range of complaints may occur. Possible symptoms may include:
- feeling of general malaise and apathy
- irritability, irritation
- learning difficulties and difficulty retaining what has been learned
- changed sleeping and eating behavior
- change in sexual behavior
- reduced social judgment
- putting objects in the mouth
- fascination with objects in the nearby environment
Some variants of encephalitis
- A.D.E.M. (or ADEM) is the abbreviation for Acute Demyelinating EncephaloMyelitis.
An inflammation of the brain (encephalitis) and the spinal cord (myelitis), in which the myelin, the protective layer surrounding nerve tissue, is broken down. It can occur as a single attack in children or as recurrent attacks. In that case it is called MDEM (multiphasic ADEM). It is also seen in older people over 65 due to infections, vaccinations or after surgery.
- Anti NMDA receptor encephalitis is an inflammation of the brain caused by the body's own antibodies directed against one's own body. This makes it an autoimmune disease in which the body produces antibodies against the NMDA receptors in the brain. The antibodies attack the body as if it were a bacteria (autoimmune reaction).
In some children with anti-NMDA receptor encephalitis, a neuroblastoma or ovarian tumor is also found. A neuroblastoma is a type of cancer that originates from the autonomic or sympathetic nervous system.
Read here or here more about anti-NMDA receptor encephalitis.
Anti-NMDA receptor encephalitis was first described by Dr. Joseph Dalmau and colleagues from the University of Pennsylvania in 2007. More information about anti-NMDA receptor encephalitis.
- Encephalitis Lethargica, also known as sleepy sickness, described by Oliver Sacks in the book Awakenings. Sleepy sickness is an atypical form of encephalitis. Between 1915 and 1926, a worldwide epidemic form of the disease occured. It attacks the brain and may cause patients to become motionless or speachless. The disease differs from Sleeping sickness which is transmitted by the tsetse fly and occurs mainly in some regions of sub-saharan Africa.
- Herpes simplex encephalitis (HSE), also called herpes encephalitis. HSE is a viral encephalitis that is usually caused by the herpes virus / cold sore virus (although a cold sore does not give an encephalitis) The frontal lobe and temporal lobe may be affected because the virus often enters through the nose.
- Brain Abscess by pus in the brain at a fixed position in the brain tissue
- HIV encephalitis, in AIDS and HIV occurs in patients with infection by the human immunodeficiency virus (HIV). Symptoms can range from listlessness, lethargy to coma. Coordination disorders and difficulty walking to paralysis (severe) cognitive symptoms including memory loss and epilepsy
- Japanese encephalitis, a virus caused by mosquitoes that are found almost everywhere in Asia. After a sting from an infected mosquito, virus development occurs both near the sting and in the regional lymph nodes. Then the virus spreads to the nervous system. Not everyone gets ill.
Complaints may include: High fever, abdominal pain, nausea, muscle pain, extreme headache, stiff neck, sometimes arm and leg pain, convulsions, hallucinations, paralysis and consciousness disturbances followed by speech and movement problems. The infection can develop into encephalitis, meningitis and / or inflammation of the spinal cord. In particular, this can occur in young children aged 3 to 6 years and the elderly. The infected person cannot infect other people, this can only be transmitted by a mosquito.
- Listeria bacterial encephalitis or meningoencephalitis:
- Listeria bacteria related encephalitis or meningoencephalitis is a serious inflammation of the brain or an inflammation of both the meninges and the brain after eating contaminated food, for example raw milk cheeses.
- Listerial brainstem encephalitis (mesenrhombencephalitis or rhombencephalitis) in which the brainstem is inflamed as a result of eating contaminated food. This can occur in healthy people. It can be very dangerous and even fatal. This form often has serious consequences and must be quickly recognized and treated with antibiotics. The bacterium 'Listeria monocytogenes' can enter the brain stem along the tenth cranial nerve, the vagus nerve, after first infecting the stomach wall. The vagus nerve branches from the brain stem to the organs (such as the intestines, stomach, heart and lungs).
- Listerial cerebritis is a rare disease (inflammation of the brain) that mainly occurs in newborns, the elderly and people with problems with the immune system.
- Listeria brain stem abscess is an abscess in the brainstem
as a result of eating contaminated food with the listeria bacteria. These abscesses in the brain stem are rare.
Q fever
- Q fever is a zoonosis.
A zoonosis (a zoonotic disease, plural: zoonoses) is an infectious disease that is transmitted between species from animals to humans (or from humans to animals). In this case, by inhaling dust or air containing the Coxiella burnetii bacteria. The bacteria can be released during the birth of lambs (goats or sheep) or calves (cows) that are infected. This may involve dust contaminated by animal feces, urine, milk or the placenta or amniotic fluid at birth.
Not everyone gets sick. Those who do become ill may have the following symptoms: fever, chills, fatigue and muscle pain, but also an inflammation of the brain (encephalitis), meningitis (aseptic meningitis) or a combination of the two, or encephalomyelitis (inflammation of the spinal cord and brain) and peripheral neuropathy, where ends of the long nerves in the body are affected.
In all cases of a combination of meningitis with a brain infection (meningoencephalitis), meningitis alone (meningitis) and in case of a nerve disorder in the feet, hands, arms or legs (peripheral neuropathy), serological tests should be carried out, because in case of Q fever a specific antibiotic treatment is required.
Acute Q fever occurs when the bacterium Coxiella burnetii can be detected in the blood (serum). The neurologist should always consider Q fever as a possible diagnosis (the differential diagnosis) in acute neurological disorders. Q fever also has a chronic form.
About 20% of people with an acute Q fever infection suffer from Q fever fatigue syndrome (QFS), which is similar to long COVID. The fatigue corresponds to neurofatigue or brain fatigue.
In addition, the following complaints have been mentioned: hypersensitivity to sensory stimuli, sleeping problems, dizziness, nausea, concentration problems and more susceptible to infections.
For information about Q fever fatigue syndrome (QFS), see here.
- Viral infection by HCoV-OC43, a seasonal coronavirus
- Creutzfeld Jacob, which is caused by a type of protein, prions,
- Tick-borne encephalitis (TBE, RSEE or CEE) is an illness that can develop after a tick bite. Infection with the TBE virus usually occurs without complaints. Those who do become ill will develop fever, headache, intense fatigue and muscle and joint pain after seven to fourteen days. Encephalitis may develop and hospitalization may be required. The complaints can progress into Lyme disease.
Since 2016, the tick-borne virus has appeared in ticks in deer in different regions in the Netherlands and Belgium.
FSME or Früh Sommer Meningo Encephalitis occurs in Russia, China, Japan, Kyrgyzstan, Kazakhstan, Mongolia, South Korea and in some parts of Europe including Austria. In the Netherlands, the Benelux and Northern Scandinavia, the tick is not (yet) infected with this FSME virus. Consider a vaccination against tick-borne encephalitis
if you stay in nature in Europe and the countries mentioned.
Lyme disease
- Lyme disease (borrelia burdorferi)
Ticks are very small creatures, but they can carry the bacteria that causes Lyme disease.
A tick bite is often contracted by walking or playing in nature. For example, in grass or shrubs where ticks live. If the tick is removed quickly, within 24 hours, the chance that Lyme disease will develop is very small. When the body is infected, the bacteria enter the bloodstream and multiply. It is important to recognize early symptoms of Lyme to stop the disease in its early stages. Consider, for example, flu-like complaints such as fever, headache, muscle pain, stiff neck and fatigue.
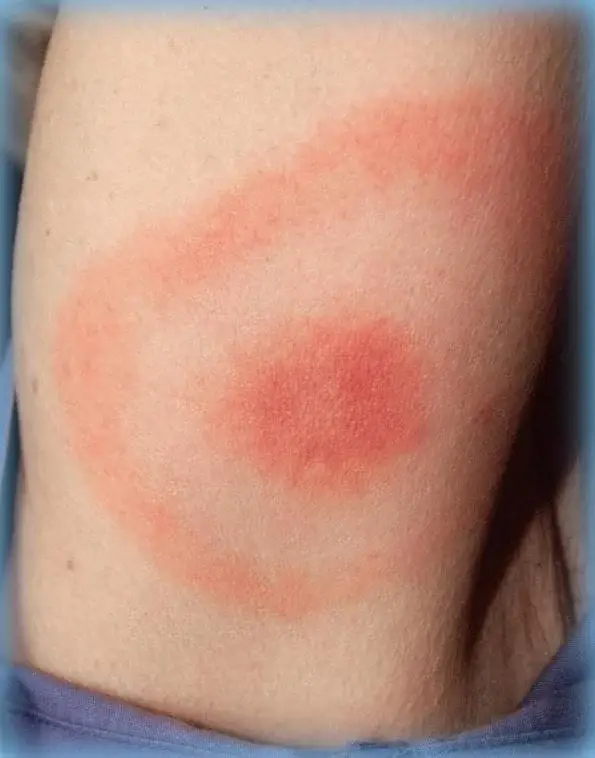
Red spot or ring - Erythema migrans
One of the first symptoms can manifest itself as a rash in the form of growing red rings, red or red-blue spot (erythema migrans or EM) within two to three weeks after the tick bite. This spot or ring occurs in approximately 60% of infected people. So not everyone gets a rash in the shape of a ring.
The ring fades from within. It is important to keep an eye on the site of a tick bite on the skin for approximately three months after the bite to see whether a red circle or spot (still) develops.
The disease can cause chronic joint inflammation, but can also cause disorders of the skin, nervous system and heart.
If the infection is present in the nervous system, the disease is called neuroborreliosis.
The consequences can be: meningitis, brain inflammation (encephalitis), eye inflammation, nerve root inflammation, facial paralysis (facial palsy/Bell's palsy).
Chronic borreliosis
If the disease symptoms persist for more than a year, it is called chronic borreliosis. Complaints often differ per person affected and per period.
Complaints
- chronic severe fatigue,
- flu-like symptoms such as fever, headache, muscle pain
- the fever is unexplained and may be accompanied by chills
- increased perspiration and/or night sweats
- swollen glands in neck, armpits and/or groin
- pain in muscles, tendons and joints
- pain in the face
- pain in the throat
- sudden double vision
- shooting pains or a numb tingling feeling in the arms
- less strength in arms, legs or torso, tingling, or pain in one or more joints
- frequent infections such as sinus infections or respiratory infections
- sometimes skin disorders or rashes in other places
- sometimes heart problems, palpitations or irregular heartbeat (skipping)
- sometimes shortness of breath or coughing
- chest pain
- joint pain
- sometimes abdominal pain with or without nausea
- changed stool pattern; constipation or diarrhea
- being able to tolerate fewer stimuli from light and sound
- ringing in the ears, tinnitus
- problems sleeping (sleeping too much or too little)
- sometimes the hormonal effect of the sex hormones changes
- sometimes cognitive disorders (difficulty thinking, planning, remembering, reading comprehension, concentrating, remembering new information and short-term memory, etc.)
- sometimes orientation problems
- sometimes word-finding problems or difficulty articulating or stuttering speech
- depression or mood swings.
Figures
In the Netherlands (17,9 inhabitants in 2024) every year 1.5 million people are bitten by a tick. Of these, approximately 27,000 people develop Lyme disease.
Of those people with Lyme disease, approximately 15,000 have long-term complaints.
More information on Lyme desease can be found here and here.
More information on encephalitis and meningitis can be found on the website of the foundation established by Jur Deitmers, 'De jongen zonder gisteren' (the boy without yesterday).
Resources
Bernit, E., Puget,J.P., Arch Janbon,, F., et al, Intern Med. 2002;162(6):693-700. doi:10.1001/archinte.162.6.693 https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/211336
Tekenbeten en de ziekte van Lyme, e-gezondheid.be | Drupal. (z.d.). Geraadpleegd op 18 januari 2015, van http://www.e-gezondheid.be/ziekte-van-lyme-uitgelegd-op-video/video/1502
Vidéo initialement mise en ligne le 17/01/2011 - 15h17 et mise à jour par Blausen (Collectief) le 09/07/2013 - 16h57En savoir plus surCohn, K. A., Thompson, A. D., Shah, S. S., Hines, E. M., Lyons, T. W., Welsh, E. J., & Nigrovic, L. E. (2011). Validation of a Clinical Prediction Rule to Distinguish Lyme Meningitis From Aseptic Meningitis.PEDIATRICS, 129(1), 46–53. https://doi.org/10.1542/peds.2011-1215
Eyskens, E., Feenstra, L., Meinders, A. E., Vandenbroucke, J. P., & Van Weel, C. (1997). Codex Medicus (10e ed.). Maarssen, Nederland: Elsevier Gezondheidszorg.
Handig die LCI-richtlijn van het RIVM. (z.d.). consulted on 18 januari 2015, from https://lci.rivm.nl/richtlijnen/japanse-encefalitis
Hersenletsel-uitleg 2013 Team hersenletsel-uitleg- laatste herziening 2019
Hersenstichting - Home [Foto]. (z.d.). Geraadpleegd op 18 januari 2015, van https://www.hersenstichting.nl/
Kayaaslan BU, Akinci E, Bilen S, Gözel MG, Erdem D, Cevik MA, Bodur H. Int J Infect Dis. 2009 Mar;13(2):e65-7. doi: 10.1016/j.ijid.2008.06.026. Epub 2008 Oct 16. PMID: 18926754
Kuks, J. B. M., Snoek, J. W., Oosterhuis, H. G. J. H., & Fock, J. M. (2003). Klinische neurologie (15e ed.). Houten, Nederland: Bohn Stafleu van Loghum.
NVN - Nederlandse Vereniging voor Neurologie :: Home [Foto]. (z.d.). consulted on 18 januari 2015, van https://www.neurologie.nl/
Richtlijn Lymeziekte. (2013, 17 juli). Geraadpleegd van https://www.rivm.nl/sites/default/files/2018-11/CBO%20richtlijn%20Lymeziekte%20definitief%20juli%202013.pdf
Wei P, Bao R, Fan Y. Brainstem Encephalitis Caused by Listeria monocytogenes. Pathogens. 2020 Aug 30;9(9):715. doi: 10.3390/pathogens9090715. PMID: 32872638; PMCID: PMC7558588.https://pubmed.ncbi.nlm.nih.gov/32872638/