MSA - Multiple System Atrophy
Multiple System Atrophy (MSA) is a progressive neurological disorder caused by the death of nerve cells in certain parts of the brain. This occurs primarily in the cerebellum, the basal ganglia, the brainstem and as a part of the brainstem called the medulla oblongata.
The cell degeneration causes problems with movement and balance. The cause of this cell degeneration is unknown.
Initially, MSA can cause problems with movement. Some people have difficulty holding their urine. Blood pressure can be so low that someone may (nearly) faint when standing up or getting out of bed or a chair.
The body's unconscious functions (autonomic functions) can also be affected. Autonomic functions include blood pressure, heart rate, sweating, and bladder control. Low blood pressure is often typical, especially when standing and walking. This condition often begins between the ages of 50 and 60. Fortunately, MSA is quite rare, affecting approximately 1 in 20,000 people. As far as we know, it is not hereditary. MSA is not contagious.
Possible Symptoms
The symptoms of MSA vary from person to person and whether it is MSA-P or MSA-C, see that chapter.
The first symptom is usually a urinary bladder problem: the patient needs to urinate more frequently, cannot urinate completely, or cannot empty the bladder at all (retention). These problems are often attributed to aging or prostate disease in men. In many men, this occurs in combination with erectile dysfunction.
There are three groups of symptoms:
1. Parkinsonism
Several conditions, such as MSA, share symptoms similar to those of Parkinson's disease, such as tremors, lack of movement, stiffness (rigidity hypokinesia), and postural abnormalities. If the symptoms are not caused by Parkinson's disease, they do not respond to the medication levodopa.
Furthermore, each of these parkinsonism disorders has its own additional symptoms, sometimes called Parkinson's Plus.
In the case of MSA, these are autonomic dysfunction and possibly ataxia.
2. Cerebellar problems
Coordination problems with movement and balance, possibly also problems with behavior and fluency.
3. Autonomic problems/autonomic dysfunction
- Bladder problems, frequent urination, inability to empty the bladder
- Erectile problems
- Feeling dizzy or fainting/problems with low blood pressure when standing or walking
- Pain around the neck or shoulders
- Constipation; Sluggish bowel movements or constipation
- Cold hands or feet
- Reduced or absent sweating.
Differences between MSA and Parkinson's disease
- Parkinson's patients often have a tendency to tremor at rest, which is rarely the case in MSA patients. In these patients, it occurs during movement.
- Autonomic symptoms (disruptions in unconscious functions) may occur in both MSA and Parkinson's disease, but in MSA autonomic symptoms play a much larger role and usually develop much earlier in the disease course, such as low blood pressure upon standing or problems with urination (incontinence or frequent urination, etc.).
-
Intellectual functions are usually preserved in MSA.
-
Other characteristics of MSA:
- A more progressive course or faster deterioration of, for example, balance problems
- Swallowing and speech problems
- A hunched posture, particularly of the head, or tilting the body to one side
- Muscle contractions
- Cold hands or feet
- Difficulty breathing, audible breathing, deep sighs, and wheezing (stridor).
- Sleep problems, such as respiratory arrest during sleep / central sleep apnea syndrome CSAS, also known as primary sleep apnea syndrome (may also occur in people with Parkinson's disease). These people may also experience impaired breathing during sleep. Snoring is not necessarily a symptom.
In many neurodegenerative disorders, including MSA, REM sleep-related disorders occur:
REM sleep-related disorder
REM sleep is dream sleep. 'REM' is an abbreviation of 'Rapid Eye Movement'.
It is called REM sleep because the eyes typically move back and forth during dream sleep. The other muscles are completely relaxed.
Someone with REM sleep-related disorder may dream very intensely and even sleepwalk because, unlike with normal REM sleep, the muscles are not relaxed.
Dreams are acted out with movements and sounds such as shouting and talking.
Sleep talking is called sleep-talking or somniloguy.
Often, a person with REM sleep disorder has injuries that he or she inflicted on him- or herself with violent movements during sleep.
A bed partner may be pushed out of bed or injured during the dream of the person with this sleep disorder.
In 70 to 80% of people with REM sleep behavior disorder, a neurodegenerative disorder (alpha-synuclein disorder) develops within about ten to twelve years.
Parkinson's disease falls under this neurodegenerative disorder, as do MSA and Lewy body dementia.
More information on this can be found here.
Two forms of MSA
There are two forms of MSA: MSA-P and MSA-C.
-
MSA-P (Parkinsonian type)
MSA-Parkinsonian type is also called Striato Nigral Degeneration (SND).
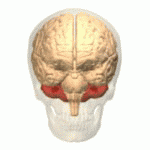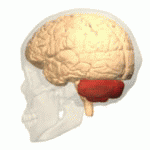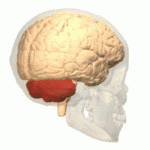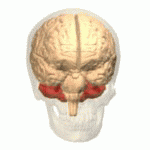
The symptoms of MSA-P resemble those of Parkinson's disease. One difference is the location where nerve cells die first. In Parkinson's disease, the dopamine-producing cells in the substantia nigra die first, and later, cells in the basal ganglia die.
The substantia nigra can be seen as the red spots in the image below:

Image source: Anatomography by Life Science Databases
In MSA-P, the disease process is precisely the opposite. First, cells in the basal ganglia (striatum) disappear, and later, cells of the substantia nigra/substantia nigra are lost.

The symptoms that occur in Parkinson's disease, such as slowness and lack of movement, also occur in MSA-P.
A difference is that in MSA-P these symptoms are not reduced by dopamine therapy. MSA-P also has several symptoms that do not occur in Parkinson's disease, such as:
- rapid disease progression
- balance disturbances, which occur early in the disease
- impaired, weak speech
- a forward-leaning posture
- autonomic nervous system disorders, particularly low blood pressure when standing and walking
MSA-C (Cerebellar Type)
Multiple System Atrophy - Cerebellar Type.
This form of MSA is also referred to as OPCA (Olivo-Ponto Cerebellar Atrophy).
In this condition, the olive nucleus in the medulla oblongata (olivo), the cerebellum, and a portion of the brainstem, the pons (ponto), are affected and shrink in volume.
MSA-C often begins with uncertain balance during movement and uncoordinated movements due to a disorder in the cerebellum. Tremors (shaking, shaking) often occur during movement. This is different from Parkinson's disease, which can occur. Speech disorders, in which the voice becomes impure and soft, usually also develop in the early stages of the disease.
MSA-C is a rare condition. It affects approximately 3.4 to 4.9 people per 100,000 inhabitants. The average age of diagnosis is between 55 and 60 years, and the average survival from the onset of motor symptoms is eight to nine years.
There are few studies on the clinical picture of MSA-C. Most studies do not distinguish between MSA-P and MSA-C.
MSA-C is not hereditary.
However, a hereditary form of ataxia does exist. This is called ADCA (ADCA stands for Autosomal Dominant Cerebellar Ataxia).
Diagnosis
An MRI scan can visualize the affected nerve cells. These brain cells shrink and can be lost, a process known as atrophy.
The diagnosis can only be made with certainty by examining brain tissue under a microscope. This cannot be done during life, only after death.
The physical examination can provide clues that MSA should be suspected. An FDG-PET scan may then provide further clues.
FDG-PET Scan
At the University Medical Center Groningen (UMCG), Laura Teune has conducted research into the FDG-PET scan that may identify early differences between neurodegenerative brain conditions that resemble each other but require different treatment.
The FDG PET scan is performed using the radioactive substance FDG (Fluordeoxyglucosis).
This allows for visualization of glucose metabolism. She discovered that different conditions show different disease-specific patterns.
Other scans can also visualize brain metabolism, such as PET scans (Position Emission Tomography) and SPECT scans (Single Photon Emission Computed Tomography). However, these scans do not reveal any abnormalities in the early stages of the disease.
When the patient's brain tissue is examined under a microscope after death, glial inclusions can be seen. These glial inclusions contain the protein α-synuclein. The presence of these inclusions in the parts of the brain responsible for movement, balance, and automatic control helps confirm the diagnosis of MSA. For more information, see also
The National Center for Biotechnology Information.
Treatment
There is currently no specific medication for MSA. Treatment for MSA involves a combination of medication, specialized devices, and therapy. The same medication used for movement disorders is often used as for Parkinson's disease. Regular medication can also be prescribed for blood pressure or bladder problems.
More information
MSA Coalition in the USA
National Institute of Neurological Disorders and Stroke
The National Center for Biotechnology Information
advertisements are not ours
Resources
Eyskens, E., Feenstra, L., Meinders, A. E., Vandenbroucke, J. P., & Van Weel, C. (1997). Codex Medicus (10e ed.). Maarssen, Nederland: ElsevierGezondheidszorg.
Hersenletsel uitleg: https://www.hersenletsel-uitleg.nl/soorten-hersenletsel-hersenaandoeningen/degeneratieve-aandoening/msa
Hersenstichting. (z.d.). Hersenstichting - Multipele systeem atrofie. Consulted februari 2015, from https://www.hersenstichting.nl/alles-over-hersenen/hersenaandoeningen/multipele-systeem-atrofie
Kuks, J. B. M., Snoek, J. W., Oosterhuis, H. G. J. H., & Fock, J. M. (2003). Klinische neurologie (15e ed.). Houten, Nederland: Bohn Stafleu vanLoghum.
Miller, D. W., Cookson, M. R., & Dickson, D. W. (2004). Glial cell inclusions and the pathogenesis of neurodegenerative diseases. Neuron GliaBiology, 1(01). https://doi.org/10.1017/s1740925x04000043
Molecular Neurology. (z.d.). Consulted februari 2015, from http://www.molgen.ua.ac.be/
msa een korte gids. (z.d.). Consulted februari 2015, from http://msa-ams.be/MSA-AMS/WAT_IS_MSA/Artikelen/2011/4/13_MSA_een_korte_gids.html
MSA Vroegtijdige hersenveroudering. (z.d.). Consulted on 1 februari 2015, from https://www.gezondheidsnet.nl/parkinson/msa-vroegtijdige-hersenveroudering
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7645310/
Ortiz JF, Betté S, Tambo W, Tao F, Cozar JC, Isaacson S. Multiple System Atrophy - Cerebellar Type: Clinical Picture and Treatment of an Often-Overlooked Disorder. Cureus. 2020 Sep 30;12(9):e10741. doi: 10.7759/cureus.10741. PMID: 33173654; PMCID: PMC7645310.Diagnosis of multiple system atrophy. Palma JA, Norcliffe-Kaufmann L, Kaufmann H. Auton Neurosci. 2018;211:15–25. [PMC free article] [PubMed][Google Scholar]
Multiple-system atrophy. Fanciulli A, Wenning GK. N Engl J Med. 2015;3:249–263. [PubMed] [Google Scholar] [Ref list]