Cerebral Infarction
Cerebral Infarction / Ischemic stroke
A cerebral infarction or "ischemic stroke" occurs due to a blockage in the blood supply through a cerebral artery (intracranial artery).
When the interruption occurs in a cerebral vein, it is called a cerebral venous sinus thrombosis.
In a stroke, a part of the brain receives insufficient oxygen and glucose because a blood vessel is blocked.
When suddenly there is not enough blood flow to certain parts of the brain, brain cells may die and functions may fail.
This may be caused by a blood clot blocking the blood vessel, a clogged blood vessel or a significant drop in blood pressure that deprives parts of the brain of blood.
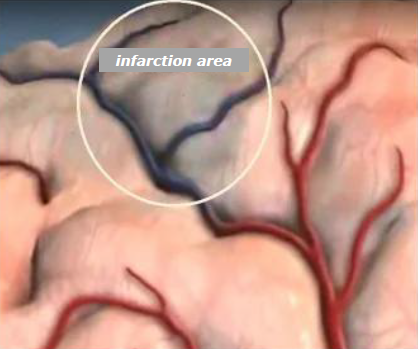

Cerebral Infarction - umbrella term: 'Stroke / CVA'
'Stroke' is a collective term for cerebral infarctions and cerebral hemorrhages. A stroke is also called CVA, which stands for Cerebrovascular Accident.
This is an 'accident in the blood vessels of the brain'.
Similarities but differences in cause
Although a cerebral hemorrhage and a stroke have different causes there is one important similarity: suddenly, some brain cells are no longer supplied with blood, oxygen and glucose.
With a cerebral hemorrhage, caused by a ruptured blood vessel, the affected area of the brain also loses its nutrients.
The affected person then experiences symptoms of loss of function, such as a paralyzed arm, a crooked mouth, or difficulty speaking.
An overview of all symptoms can be found on the stroke recognition page.
The various causes of a stroke
A stroke may be caused by:
- A blood clot from elsewhere in the body (embolism), often caused by a heart rhythm disorder (atrial fibrillation)
- A blood clot from an unhealthy blood vessel (thrombus)
- Atherosclerosis
- Inflammation of the inner lining of blood vessels (vasculitis)
-
Clotting disorders, such as lupus anticoagulans or APS, SLE (systemic lupus erythematosus), Thrombotic Thrombocytopenic Purpura (TTP), Paroxysmal Nocturnal Hemoglubinuria (PNH), Essential Thrombocythemia (ET); a myeloproliferative disorder.
-
Vascular disorders, such as lacunar infarction or diseases like CADASIL or RVCL.
-
Watershed infarction: a cerebral infarction that occurs in the border area between two major cerebral arteries. This can be caused by insufficient blood flow due to blood loss, a drop in blood pressure, micro-embolisms, or severe narrowing or occlusion of the carotid artery.
-
Women who take birth control pills have a higher risk of a cerebral infarction, according to researchers from UMC Utrecht and Leiden University Medical Center (LUMC). They have discovered a gene that partly determines this risk. Variations in the coagulation factor XIII gene are associated with an increased risk of stroke. See https://pubmed.ncbi.nlm.nih.gov/18006701/
There are also studies that conclude: "Low estrogen oral contraceptives do not appear to increase the risk of stroke."
Unfortunately, a cause is not always found.
A TIA (Transient Ischemic Attack) is a temporary blockage in a blood vessel in the brain. It is also called a mini-stroke. If the symptoms do not subside after 24 hours it is called a cerebral infarction. However, many people experience prolonged symptoms after a TIA.
That is why we created a separate page about TIA.
A stroke due to an irregular heartbeat / heart rhythm disorder
The heart has four hollow chambers: the left and right atriums at the top of the heart, and the left and right ventricles at the bottom.
The left side of the heart processes oxygen-rich blood and the right side processes oxygen-poor blood. The ventricles provide the heart's pumping function, while the atria serve as a collecting reservoir.

Ventricular fibrillation is a serious heart rhythm disorder that may lead to cardiac arrest.
Atrial fibrillation is a common heart rhythm disorder, but it is often the cause of a stroke.
The heart beats irregularly and rapidly, with varying degrees of intensity. It feels like the heart is racing.
This is called an irregular pulse. The heart beats 150 times per minute or faster. A normal resting heart rate is 60 or 70 beats per minute.
Symptoms that someone with atrial fibrillation may experience include:
- palpitations
- pounding heart
- fatigue
- reduced ability to exert themselves
- shortness of breath
- sweating
- chest pressure or chest pain
- dizziness
- fainting
- heart failure.
These symptoms occur when the heart beats faster than 120 beats per minute. Atrial fibrillation can also occur at beats less than 120 per minute and in that case, the person usually doesn't experience much discomfort or discomfort.
A common risk of atrial fibrillation, besides heart failure, is stroke. Because the heart's atria beat too rapidly and irregularly, blood cannot be pumped properly. This can cause blood to stagnate, usually in the left atrium, and clot.
When a blood clot breaks loose, it is pumped through the body via the powerful blood flow of the large arteries. The clot travels until it reaches a smaller artery where it becomes lodged. Like a cork, it suddenly and completely blocks the artery. A blood clot can also form directly at the site of the blockage (thrombosis or thrombus), which may lead to a stroke.
Atrial fibrillation usually does not directly cause a heart attack, but it can increase your risk of serious heart problems. Because blood flows less efficiently through the heart, there is an increased risk of blood clots. If such a clot breaks loose and blocks a blood vessel in the heart, it can cause a heart attack. Atrial fibrillation can eventually even lead to vascular dementia.
Therefore, if a doctor diagnoses atrial fibrillation, he or she will prescribe anticoagulant medication. It is therefore recommended to have your blood pressure checked at least once a year.
If you experience symptoms of an irregular heartbeat it is advisable to consult a doctor. It could be a harmless, transient heart rhythm disorder, but it could also be more serious, with the symptoms we mentioned with atrial fibrillation.

Recognize a stroke!
Time loss is brain loss

Call emergency services immediately
Symptoms
Although the cause differs the symptoms of a cerebral hemorrhage and a stroke are the same.
A stroke occurs quickly and unexpectedly and can be recognized by the following symptoms:
- facial paralysis (e.g., a crooked mouth)
- Slurred speech and thinking
- Tingling
- Vision disturbances or loss, such as double vision, blurred vision, or
- one-sided visual field loss
- Severe headache
- Dizziness and balance problems
- Paralization, numbness, or loss of strength
- Nausea
Women often exhibit atypical symptoms such as disorientation, confusion, and loss of consciousness.
If in doubt, err on the side of caution and call the emergency number!
An overview of all symptoms can be found on the stroke recognition page.
Of all strokes:
- 80% are cerebral infarctions
- 20% are cerebral hemorrhages
A stroke affecting the right hemisphere of the cerebrum results in paralysis on the left side of the body, and vice versa. A stroke affecting the left hemisphere of the cerebellum results in paralysis on the left side of the body, and vice versa. For more information see here and here.
Treatment of a stroke
In the case of a stroke caused by a blood clot thrombolysis may be an option, provided it occurs within 4.5 hours of the first symptoms of loss of function. Symptoms such as paralysis of an arm or leg, or difficulty speaking, may indicate this.
Thrombolysis involves administering a medication through an IV that dissolves the blood clot.
This treatment may limit the damage after a stroke.
More information about trombolysis here.
Thrombolysis is a treatment for a small group of people who suffered a stroke
A prerequisite is that thrombolysis must be administered within 4.5 hours.
The chance of recovery decreases, and the risk of complications (especially severe bleeding) is relatively high.
In addition, the neurologist uses a CT scan to determine whether a cerebral infarction or a cerebral hemorrhage has occurred. If the CT scan shows signs of bleeding, thrombolysis is not possible.
Thrombolysis is not performed if
- the symptoms of failure subside rapidly or are minor
- the CT scan reveals a very large stroke
- the blood pressure is too high
- the glucose level is too low or too high
- there is a high risk of bleeding, for example, due to the use of anticoagulants or heparin
- the person has previously had a bleeding event in or around the brain
- the person has had major surgery in the two weeks before the stroke
- the person has had a heart attack or bleeding in the gastrointestinal or urinary tract in the three weeks before the stroke.
Thrombectomy
A thrombectomy is a medical procedure to remove a blood clot from a blood vessel. This procedure is often performed for people who have suffered a stroke due to a blockage in the blood supply to the brain.
During the procedure, a thin tube, a catheter, is inserted into the blood vessel. The clot is then gently dislodged and removed. This helps restore blood circulation and prevents further damage to the brain.
Thrombectomy can be life-saving for people with an acute stroke and is usually performed in well-equipped and knowledgeable hospitals.
This procedure can usually be performed within six to eight hours of the onset of symptoms.
It is important that a team of neurologists evaluate the patient's situation to determine the best treatment option, depending on the specific circumstances and the patient's medical history.
Thrombolysis or thrombectomy?
The choice between thrombolysis and thrombectomy depends on several factors, such as the type of stroke, the time since symptoms began, and the patient's health.
Cerebral Vessels
On the Cerebral Vessels page we explain all the consequences of each blood vessel involved in a stroke. This includes a schematic overview of the consequences and the flow areas of each artery.
A video about a stroke
Watch the particularly impressive animation about a stroke here.
advertisements are not ours