Stroke - CVA
A stroke, sometimes referred to as a cerebrovascular accident (CVA), cerebrovascular insult (CVI), or colloquially brain attack, is the loss of brain function due to the poor blood supply to the brain.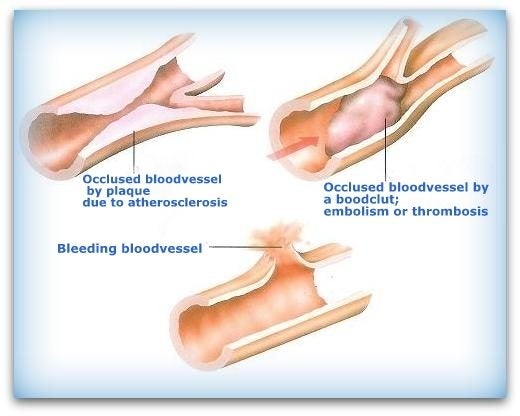
At a stroke suddenly a part of the brain cells stop working. The affected area of the brain cannot function normally, which might result in an inability to move one or more limbs on one side of the body, failure to understand or formulate speech, or a vision impairment of one side of the visual field.
TYPES OF STROKE
- Hemorrhagic Stroke
- A bloodvessel in the brain ruptures and bleed, causing brain cell death.
- Occurs in 10-15% of stroke patients.
- Ischemic Stroke
- A blood clot forms in a main artery, blocking and reducing blood supply, causing brain cell death.
- Occurs in 85-90% of stroke patients.
A stroke can occur in several ways:
- Due to a temporary shortage of blood in certain brain cells: TIA.
- By persistently occluded vessel in the brains: ischemia ( caused by either blockage of a blood vessel via thrombosis or arterial embolism, cerebral infarction or a build up of plaque in an artery due to atherosclerosis, sometimes beacause of an autoimmune disease like Anti-phospholipid Syndrome; APS and lupus anticoagulant)
- By bleeding blood vessel in the brains: cerebral hemorrhage. Either by directly into the brain or into the subarachnoid space surrounding brain tissue.
At a stroke in the right hemisphere, the left side of the body is paralyzed, and vice versa.
HOW TO RECOGNIZE A STROKE FAST?
For a stroke for the same as a heart attack, the faster the better in the hospital. By powerful anti-clotting drugs, the closure of the artery in the brains can be resolved, so the damage is limited in certain cases. For bystanders, it is important to identify quickly a stroke and to call the emergency number of the country.

CALL IMMEDIATELY for help!
F.A.S.T. is an easy way to remember the sudden signs of stroke. When you can spot the signs, you'll know that you need to call the national emergency number 911 in USA, 999 in UK 112 in Europe right away. F.A.S.T. is:
| F |
Face Drooping – Does one side of the face droop or is it numb? Ask the person to smile. Is the mouth crooked while the person is smiling? Ask to smile and show the teeth
|
| A |
Arm Weakness – Is one arm weak or numb? Ask the person to raise both arms. Does one arm drift downward? It is important for the person, to keep the eyes closed.
|
| S |
Speech Difficulty – Is speech slurred? Is the person unable to speak or hard to understand? Ask the person to repeat a simple sentence, like "The sky is blue." Is the sentence repeated correctly? Ask simple questions What day of the week is it today? Where are we now? Note slurred and confused speech. |
| T |
Time to call the emergency number– If someone shows any of these symptoms, even if the symptoms go away, call and get the person to the hospital immediately. Check the time so you'll know when the first symptoms appeared. |

STROKE VIDEOS:
TREATMENT OF CEREBRAL INFARCTION
For a stroke a treatment called thrombolysis, is possible within 4.5 hours after the first failure symptoms, such as paralysis of the arm or leg, or trouble talking.
When you get an thrombolysis you'll get an IV with clot-dissolving drugs.
This treatment reduces the damage after a stroke. Thrombolysis is a treatment for a limited group of patients with cerebral infarction.
The first condition is that thrombolysis should occur within 4.5 hours. The chance of recovery is getting smaller and the risk of complications (mainly bleeding) is relatively large.
Reviews the neurologist on the basis of a CT scan if there is a stroke or brain hemorrhage. If the CT scan shows signs of bleeding, thrombolysis is not possible.
Thrombolysis is not further performed if:
- the deficits rapidly reduce
- a CT scan shows a very large stroke
- the blood pressure is too high
- the bloodsugar gets too low or too high
- there is a high risk of bleeding, for example, by the use of anti-coagulant or heparin
- someone has had a bleeding in or around the brains previously
- someone has had a major surgeryin the two weeks before the stroke
- someone has had a heart attack or bleeding in the gastrointestinal tract or urinary tract in the 3 weeks before the stroke
TIA / TRANSIENT ISCHEMIC ATTACK
A TIA is a blockage of a blood vessel in the brains, even causing a shut down. Usually by a tiny blood clotting. A TIA is a light stroke, a mini-stroke, wherein the embolism (thrombus) in the artery is shutting down the brains of blood supply for a short period of time.
Once you have had a TIA, it increases the risk of a second stroke. TIA should be seen as a warning.
The failure may take a few minutes, but also hold on for half an hour.
Someone with a TIA may have a hanging mouth or cannot speak properly. Sometimes he/ she can not move his / her arm.
If you think someone has a TIA or stroke (both have the same symptoms), you can ask if the person wants to lift his arm upwards. Ask him to show the teeth or have him anything to say. If this fails, you better call the emergency number.
The symptoms of a TIA usually disappear quickly and the person will have no permanent injuries. Often the symptoms disappear after 20 minutes.
Yet a TIA is indeed dangerous, because it is sometimes followed by a stroke or cerebral infarction and that has much more serious consequences than a TIA.
If the symptoms dissapear within 24 hours we speak of a TIA. If the symptoms lasts longer than 24 hour it is a stroke.
The limit of 24 was chosen quite arbitrarily. What matters is that a TIA is gone after a short time, while a stroke over a longer period. Do you have residual symptoms then there is a cerebral infarction.
Coagulation-resistant medication and avoiding risks for an artery disease may make the risk of a second TIA considerably smaller. In some cases, treatment of a narrowed carotid artery may follow.
Causes of a TIA :
- arteriosclerosis
- arrhythmias
SEE TIA VIDEO WITH THIS LINK:
STROKE TREATMENT VIDEO:
CAUSES OF A HEMORRHAGIC STROKE
The cause of a hemorrhagic stroke is a tear in a blood vessel. Blood flows in or around the brains. The blood accumulates and pushes the brain tissue away.
As a result, the brain tissue get damaged. A stroke can be caused by a flaw in the blood vessels (aneursyma) or malformation of the blood vessels (arteriovenous malformation AVM) or high blood pressure. Learn more...
A bleeding may also be caused by an accident.
An aneurysm is a weak spot in a blood vessel that occurs throughout life. With age the aneurysm grows slowly into a bubble. High blood pressure and arteriosclerosis accelerate this process. If the aneurysm ruptures it creates a hemorrhage.
Learn more....
VIDEOs OF HEMORRHAGIC STROKE :
THE EFFECTS OF A STROKE / CVA
The effects of a stroke stroke can be great:
Neurological effects as a cripple on one side of the body (hemiparesis), or an arm or leg, or even a complete paralysis (hemiplegia), but also a face half palsy (facial palsy). Often in the early stages the muscle weakness is characteristic. Later on often are seen coordinationproblems and spontaneous contraction (spasm or spasms) of the muscles which can be very annoying.
- Loss of sensory registration. The sense doing it yet, but the receipt by the brains is disrupted; sometimes reinforced, sometimes less.
- Epilepsy
- Aphasia; Usually when the hemorrhage was in the left hemisphere, because in 90% of humanity the language-area is situated there. Current research suggests that right-handers and about 70% of left-handers utilise the left brain for speech.
The aphasia (a = not, phasia = speaking) can present itself as difficulty in speaking (Broca's aphasia) as also in a disrupted language comprehension (listening and reading) Wernicke's Aphasia.
Often both forms occur at the same time = global aphasia. Aphasia is an acquired communication disorder that impairs a person's ability to process language, but does not affect intelligence. Aphasia impairs the ability to speak and understand others, and most people with aphasia experience difficulty reading and writing.
- Impairment in spatial information. Often this will happen after a hemorrhage in the right hemisphere. Getting lost in rooms, buildings, street etc. Not recognizing areas. Struggling with new info.
- Invisible effects as cognitive disorders. See also the list on the subpage "invisible effects of brain injury"
Hemiparesis and hemiplegia
Hemiparesis refers to one-sided ('hemi') weakness ('paresis') The words 'hemiparesis' and 'hemiplegia' are used next to each other in practice.
In fact, 'plegia' means complete paralysis and 'paresis' means partial paralysis;
On one side of the body both arm and leg and face can be affected. It may also be that only the arm is affected, or only the leg or facial muscles. Hemiparesis affects roughly 80 percent of stroke survivors, causing weakness or the inability to move one side of the body.
At a stroke in the right hemisphere one is left paralyzed and vice versa. Paralysis is not always the case. The speech and language center is located in the left hemisphere in right-handers.
A stroke in the left hemisphere often gives an impairment in the use of language (both speaking and understanding).
A stroke in the right hemisphere can cause paralysis on the left side, but also often results only in other, less immediately striking disorders.
Striking or not, they can indeed very prohibitive for everyday life.
As more brain tissue is damaged, the consequences are more serious.
Hemiparesis refers to one-sided ('hemi') weakness ('paresis') The words 'hemiparesis' and 'hemiplegia' are used next to each other in practice.
In fact, 'plegia' means complete paralysis and 'paresis' means partial paralysis;
On one side of the body both arm and leg and face can be affected. It may also be that only the arm is affected, or only the leg or facial muscles.

Resources:
hersenletsel-uitleg.nl ,National Aphasia Association NY, , National Institute of Neurological Disorders and Stroke (NINDS).
Coping with brain injury Palm, Frontiers in neuroloy, neurotrauma, brain health board in boxers and soccer, Left brain right brain Springer & Deutsch, JBM Kuks, J. W. Pike, H.J.G.H. Oosterhuis. Clinical Neurology 15th Edition, Bohn Stafleu Of Loghum, Wood, 2003, ISBN 90-313-4028-6