Brain Injury by oxygen deficiency or lack of oxygen




Causes of oxygen deficiency
A lack of oxygen in the brain can occur after:
- Cardiac arrest (due to infarction / cardiac arrhythmia) and after prolonged resuscitation. It can also be caused by a heart attack or heart valve disease.
See also our page on heart patients or brain injury patient
- Respiratory arrest, for example in the event of (near) drowning, suffocation or choking
- Prolonged epileptic seizure / status epilepticus
- Poisoning (smoke or toxic substances) see also intoxication
- Serious lung problems
- Attempted strangulation
- Attempted hanging (suicide attempt)
- Choke challenge, choking games
- Being buried (avalanche, rubble, earth, sand, etc.)
- Asphyxia literally means 'not breathing' This leads to a lack of oxygen in the baby around birth, which can damage various organs in the body. See further down this page for more information. This lack of oxygen can lead to the same consequences as a lack of oxygen later in life
- Choke challenge, choking games
- Using too much laughing gas. Laughing gas blocks the glutamate receptor, a neurotransmitter that is involved in all kinds of processes in the brain. It causes a temporary lack of oxygen in the brain. With more intensive use, the damage can increase. A vitamin B12 deficiency can also lead to failure in the spinal cord. Leave laughing gas where it belongs: with the doctors to anesthetize you.
Officially, a CVA (stroke) is also a circulatory disorder of the central nervous system. In a stroke, however, the oxygen deficiency is limited to a part of the brain.
Three minutes of OXYGEN emergency supply
The heart pumps oxygenated blood throughout the body. Two pairs of large arteries branch throughout the brain. They bring a continuous flow of oxygen and glucose. This process provides all the energy to keep brain cells alive and functioning.
After three minutes
When there is a lack of oxygen in the brain, the brain first increases the blood supply.
In serious circumstances, this is not always sufficient. The brain has an emergency energy supply for about three minutes.
This also means that if resuscitation is not started within two minutes in the event of cardiac arrest, that supply will quickly be depleted. The result can be that damage occurs everywhere in the brain with
cognition and memory problems.
If the lack of oxygen has lasted longer, the memory problems become worse and those affected often have a form of
aphasia. In addition, all kinds of motor abnormalities can occur, such as tremors and/or paralysis.
A lack of oxygen from three to nine minutes can result in irreversible brain damage! In case of a cardiac arrest a CPR (Cardiopulmonary resuscitation) is best started within two minutes.
An ischemic stroke occurs when a part of the brain die because of a blocked arteria which lead to a partial lack of oxygen.
Damage in brain areas
The most vulnerable areas of the nervous system are:
- Cerebral cortex, especially around the central sulcus. This is the central groove that vertically separates the frontal lobe from the brain areas behind it. Indicated in the image below with the red line:
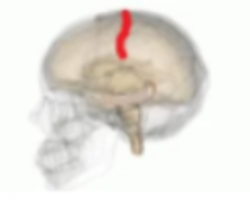






- Spinal cord
Brain cells, kidney cells and liver cells are sensitive to oxygen deficiency.
Oxygen deficiency causes damage everywhere
Damage after oxygen deficiency occurs everywhere where blood normally flows. This is also called diffuse brain damage. Parts of the brain die, spread throughout the entire brain and this process continues as the minutes pass.
The cerebral cortex and the temporal lobe (near the temples) in particular are sensitive to oxygen deficiency, which can quickly damage cognition and memory.
An oxygen deficiency of three to nine minutes leads to irreversible brain damage.
NB! In the event of cardiac arrest, it is therefore best to start resuscitation within two minutes.
Possible consequences
Brain death
Coma
Vegetative state
Minimally conscious state (MBT) / Low conscious state (LBT)
Delirium
Neurological deficit
- Paresis, muscle weakness, especially of the arms
- Dystonia
- Spasticity
- Parkinsonism, combination of symptoms that occur in
Parkinson's disease - Spinal cord damage
- Cortical blindness
- Incontinence
- Walking problems
- Speech difficulties
- Epilepsy
More information: Neurological deficit
Cognitive disorders
- Changed personality
- Memory problems
- Disorientation (place, person and/or time)
- Concentration problems
- Confusion
- Fatigue
More information: Cognitive disorders
The difference in consequences is significant
The consequences of oxygen deficiency in the brain differ per person and per situation. One person will have mild residual symptoms, while another will no longer have any sense of life.
Nowadays, there is more attention for the cognitive damage that people suffer after oxygen deficiency. For example, cognitive screening is performed more often, because memory in particular is affected so quickly.
Brain damage after cardiac arrest, infarction and arrhythmias
It is estimated that in eight out of ten successful resuscitations, i.e. the person survives, the patient becomes comatose and suffers brain damage. In addition to being a heart patient, this person is also a brain damage patient.
The question now is actually: to what extent do you call the resuscitation successful?
Prognoses depend on circumstances such as temperature (heat or cold), speed of starting resuscitation, expertise of the emergency worker(s), and the location of the person with cardiac arrest.
Is the person being resuscitated in a remote area or already in (near) a hospital?
For a patient who is in poor condition, with many additional complaints, the chance of success is considerably lower than for someone in good condition.
Failure to resuscitate means that the patient will die quickly. The patient will be unconscious within seconds.
Neurological problems after cardiac arrest
Neurological results of cardiac arrest survivors vary considerably, from complete recovery to life in a vegetative state.
Not only does oxygen and glucose deficiency cause damage to the brain. The loss of blood flow due to cardiac arrest and the subsequent restarting of the heartbeat, by means of cardiac massage or an AED shock, also causes damage to the brain.
In order to limit damage to the brain and organs as much as possible, the patient is cooled to a temperature of 33ºC and kept at this temperature for a day.
Neurologists are often asked to assess coma patients after cardiac arrest, in an attempt to predict the degree of recovery that may occur.
Patients who recover quickly after resuscitation usually do not pose a problem for the prognosis.
Patients with a short circulatory arrest who suffered from a milder degree of oxygen deficiency in the brain show characteristics of a
reversible metabolic encephalopathy. Reversible means that recovery can occur.
Recovery after a short coma
If there is a coma and it lasts a maximum of a few hours (on average twelve), patients show some physical, sensory and intellectual problems upon awakening. They may be confused or experience a gap in memory of a few hours to days. Recovery is usually quick and complete.
Incomplete recovery after severe oxygen deficiency
There are also patients with severe systemic anoxia-ischemia (anoxia = no oxygen / ischemia = oxygen deficiency in the blood). This causes structural damage, comparable to damage after a stroke. Patients in this group have usually been in a coma for at least twelve hours and upon awakening have persistent sensory, intellectual and motor problems, either in one area of the brain (focal) or in multiple areas (multifocal) or spread throughout the brain (diffuse injury). Recovery is often incomplete and slow.
Severity of disabilities
Brain damage after cardiac arrest can cause changes in movement, perception, feeling and thinking.
Some patients are later able to lead an independent life at home despite remaining neurological problems (moderately disabled).
Some can even work again. Possibly with adjusted working hours and rest breaks.
Cognitive disorders can be subtle and often not immediately visible. However, these disorders can significantly affect the patient's daily activities, participation in society and quality of life.
Other survivors of resuscitation have become severely disabled and dependent on help. They usually live in a nursing home. Patients with greater diffuse damage (damage throughout the brain) can end up in a state of being awake but unconscious (vegetative state) or are brain dead.
Lance-Post-Adams Syndrome (LAS) or Post-Hypoxic Myoclonus (PHM)
Lance-Adams syndrome (LAS), also known as post-hypoxic myoclonus (PHM), is a rare neurological complication that occurs after a period of hypoxia (oxygen deficiency) in the brain.
It usually occurs in people who have survived cardiac arrest and regained consciousness after a period of time.
These people develop muscle twitches or jerks (myoclonus) days, weeks, or even months after resuscitation.
Lance-Adams syndrome can also occur after:
- a severe attack of bronchial asthma (status asthmaticus)
- asphyxiation
- pulmonary embolism
- a suicide attempt by hanging or attempted strangulation
- any other disruption of the oxygen supply to the brain.
Symptoms
- Motor problems: Patients may experience involuntary and irregular movements, tremors, and muscle twitches/spasms.
These are often described as dystonic movements.
Such involuntary muscle contractions are called myoclonus. "Myo" means muscle, and "clonus" means spasm. Myoclonus often involves abnormally increased excitability of the cerebral cortex.
It appears to be caused by oxygen damage to the basal ganglia, a group of brain nuclei involved in movement.
- The syndrome is often accompanied by difficulty articulating when speaking (dysarthria). This is caused by the fact that mouth and tongue muscles may also be affected. A person with the LAS syndrome has a high risk of choking. Making fine movements may be very difficult. The more the person tries to make precise movements, the more muscle twitches may occur. Relaxation and rest often prove helpful. Experiencing muscle twitches is extremely tiring, and people with oxygen damage to the brain are often already at risk of severe overstimulation and neurofatigue (brain fatigue).
- Cognitive problems such as difficulty with memory, thinking, difficulty concentrating, and changes in judgment.
- Sleep disturbances: Sleep problems may also occur, which can contribute to overall fatigue and cognitive problems.
- Neurological problems as listed on this page
The syndrome is named after the authors who described it in 1963: Lance and Adams.
They called it "chronic posthypoxic myoclonus," a long-term, disabling neurological disorder that occurs in survivors of anoxia
(anoxia is a lack of oxygen in tissues and organs). More information can be found here.
Acute PHM
If the muscle twitches occur within 12 hours of cardiac arrest or other brain oxygen interruption, while the person is still in a deep coma, it is called acute posthypoxic myoclonus (acute PHM), posthypoxic myoclonic status epilepticus, or acute posthypoxic myoclonus.
MSE
A similar picture is seen in the epileptic seizures of myoclonic status epilepticus (MSE), also a consequence of a lack of oxygen to the brain, usually following resuscitation. In MSE, the muscle twitches, or myoclonic seizures, last longer than 30 minutes.
Simultaneous electroencephalography (EEG) and muscle-nerve imaging (EMG) can distinguish between MSE and LAS. In LAS, a specific EEG pattern of vertex spike-wave discharges is observed
with a continuous background. More information about the differences
see halfway down this page.
An experience from someone with Lance Adams Syndrome
"Today was a day I had convulsions that lasted more than 24-72 hours. I shake nonstop, all day long except when I sleep. On these days, I can't walk, eat, shower, or even brush my teeth.
A nerve conduction study showed nothing. My nerves and nerve pathways function perfectly.
On the days when the shaking is at its worst, I try to stay in bed, because there's nothing I can do about these muscle twitches. I don't eat anything because I feel like even my stomach is turning and giving me stomach upset. Sometimes there's a seven-day break (interval) between attacks. Later, it happened every two and then every three weeks."
See the video
Difference between anoxia, hypoxia, asphyxia and ischemia (ischemia)
Brain damage due to oxygen deficiency is called postanoxic and/or posthypoxic encephalopathy.
The terms anoxia and hypoxia are used interchangeably but are essentially different from a medical perspective. The word asphyxia is only used for oxygen deficiency around the time of birth.
- Anoxia: a total lack oxygen deficiency in tissues and organs.
- Hypoxia: reduction or inadequate flow of oxygen in the blood.
- Asphyxia: oxygen deficiency around the time of birth. It literally means not breathing. It can be caused by a placental abruption or problems with the blood flow to the placenta such as a placental infarction.
- Ischemia (sometimes still spelled as ischaemia) is insufficient blood flow and reduced blood supply to organs and body tissues, resulting in a shortage of oxygen and glucose.
NB! Damage is not always visible on an MRI scan. Demonstrable abnormalities on an MRI scan may sometimes only become visible after several days, but they may also disappear again.
Is it wise to resuscitate or not? Be prepared!
If resuscitation is not performed, the patient will die quickly.
Studies in humans show that someone without blood flow to the brain loses consciousness within 4 to 10 seconds.
That is why you and your loved ones should always ask yourself the question: Resuscitation or not?
In order to make a good decision, it may be advisable to have a conversation with your treating (family) doctor, the nurse and your family.
Your treating doctor can tell you more about your situation from a medical point of view. You can discuss how to make a good choice with nurses, spiritual counselor or ethicist and of course your family.
Resuscitation? Then also take a resuscitation course.
Download an resuscitation app.
Make sure your phone is on speakerphone so that you can call emergancy telephone number at the same time.
Know that brain cells die after just three minutes of cardiac arrest.
Talk about it with your loved ones and make a choice together: whether or not to resuscitate.
One of the best-known neuropsychologists in the Netherlands, Jenny Palm, can get excited about the naive assumption that resuscitation, as a widely practiced popular skill, would save lives.
"People enter the hospital as heart patients and leave the hospital as brain injury patients."
She states the following in an interview:
"There is a resuscitation hype going on, the manly saving of people's lives after a cardiac arrest, without the question being asked how far you should go.
We now know that 95% of such resuscitations have a very poor outcome. There is all kinds of research that attributes the highest chance of success in resuscitation to intervention in the operating room, during an operation.
The interval between cardiac arrest and successful resuscitation is the shortest in the operating room. Everywhere else, resuscitation is performed with sometimes dangerously long intervals, which greatly reduces the chance of a full and complete recovery.
People are encouraged to take resuscitation courses so that at some point they can save their partner or someone else. The effect of this is twofold: those who cannot resuscitate are saddled with a feeling of guilt, but so are those who have resuscitated, when they often have to conclude that the person they have saved saved and then goes through life with serious brain damage.
Quality of life should be the criterion. As long as someone is recovering, nothing is too much to let the patient regain what has been lost with all kinds of tricks, but after that it is over and the patient and the entire social system around him or her can figure it all out for themselves".
What is the view of researchers?
Drop-down menu:
Overview and insight
Neurologist Dr. G. Roks made the overview below about the duration of the oxygen deficiency and the damage to both the brainstem and cerebral cortex. He also made a Powerpoint presentation (in Dutch) about Postanoxic encephalopathy. Available for download below.
A neuropsychological evaluation and/or cognitive rehabilitation is recommended. Visually invisible damage is also examined.
The document below provides information in English.
Resources
Hersenletsel-uitleg.nl
https://www.hersenletsel-uitleg.nl/soorten-hersenletsel-hersenaandoeningen/zuurstoftekort
Argent, D. E., & Cope, D. H. (1956, 17 maart). Cerebral hypoxia: aetiology and treatment. British Medical Journal, pp. 593–598. Consulted from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1979171/
Beesems SG, Blom MT, van der Pas MH, Hulleman M, van de Glind EM, van Munster BC, Tijssen JG, Tan HL, van Delden JJ, Koster RW. Comorbidity and favorable neurologic outcome after out-of-hospital cardiacarrest in patients of 70 years and older. Resuscitation. 2015 Sep;94:33-9. doi: 10.1016/j.resuscitation.2015.06.017. Epub 2015 Jun 25. PMID: 26116780.
Berek, K., Jeschow, M., & Aichner, F. (1997). The Prognostication of Cerebral Hypoxia after Out-of-Hospital Cardiac Arrest in Adults. European Neurology, 37(3), 135–145. https://doi.org/10.1159/000117426
Cronberg T, Greer DM, Lilja G, Moulaert V, Swindell P, Rossetti AO. Brain injury after cardiac arrest: from prognostication of comatose patients to rehabilitation. Lancet Neurol. 2020;19:611–622De Nederlandse Hartstichting. (z.d.). Oplossingen voor een sterk hart | Hartstichting. Consulted on 7 juni 2013, van https://www.hartstichting.nl/
Fischer M, Bockhorst K, Hoehn-Berlage M, Schmitz B, Hossmann KA. Imaging of the apparent diffusion coefficient for the evaluation of cerebral metabolic recovery after cardiac arrest. Magn ResonImaging. 1995;13:781–790.Geocadin RG, Callaway CW, Fink EL, Golan E, Greer DM, Ko NU, Lang E, Licht DJ, Marino BS, McNair ND, Peberdy MA, Perman SM, Sims DB, Soar J, Sandroni C, American HeartAssociation Emergency Cardiovascular Care C Standards for studies of neurological prognostication in comatose survivors of cardiac arrest: a scientific statement from the American Heart Association. Circulation.2019;140:e517–e542.
Eyskens, E., Feenstra, L., Meinders, A. E., Vandenbroucke, J. P., & Van Weel, C. (1997). Codex Medicus (10e ed.). Maarssen, Nederland: Elsevier Gezondheidszorg.
Ik wil nooit beroemd worden [Film]. (2010, 29 juli). Consulted on 7 juni 2013, van https://www.2doc.nl/documentaires/series/hollanddoc/2007/Ik-wil-nooit-beroemd-worden.html
Koenig MA. Brain resuscitation and prognosis after cardiac arrest. Crit Care Clin. 2014 Oct;30(4):765-83. doi: 10.1016/j.ccc.2014.06.007. Epub 2014 Jul 30. PMID: 25257740.Kuks, J. B. M., Snoek, J. W., Oosterhuis, H. G. J. H., & Fock, J. M. (2003). Klinische neurologie (15e ed.). Houten, Nederland: Bohn Stafleu van Loghum.
Madl, C., & Holzer, M. (2004). Brain function after resuscitation from cardiac arrest. Current Opinion in Critical Care, 10(3), 213–217. https://doi.org/10.1097/01.ccx.0000127542.32890.faNg YY, Wah W, Liu N, Zhou SA, Ho AF, Pek PP, Shin SD, Tanaka H, Khunkhlai N, Lin CH, Wong KD, Cai WW, Ong ME; PAROS Clinical Research Network. Associations between gender and cardiac arrest outcomes inPan-Asian out-of-hospital cardiac arrest patients. Resuscitation 2016;102:116–121 Rossen R, Kabat H, Anderson JP. Acute arrest of cerebral circulation in man. Arch Neurol Psychiatr. 1943;50:510–528.
Palm, J. (2012). Omgaan met Hersenletsel. Assen, Nederland: Van Gorcum.
Roks, G. (2012, 7 november). Postencefalitische encephalopathie,neurologische aspecten. Consulted on 13 juni 2013, van https://www.slideserve.com/barb/postanoxische-encephalopathie-neurologische-aspecten Sandroni C, Cronberg T, Sekhon M. Brain injury after cardiac arrest: pathophysiology, treatment, and prognosis. Intensive Care Med. 2021 Dec;47(12):1393-1414. doi: 10.1007/s00134-021-06548-2. Epub 2021 Oct 27. PMID: 34705079; PMCID: PMC8548866.
Verenso, NHG, & V&VN. (2013, 4 april). Reanimatie - Verenso. Consulted on 7 juni 2013, van https://www.verenso.nl/kwaliteit-en-richtlijnen/richtlijnendatabase/reanimatie-1
www.bosk.nl/cerebrale-parese/wat-is-cp/oorzaken/. (z.d.). Consulted from https://www.bosk.nl/cerebrale-parese/wat-is-cp/oorzaken/
Wachelder EM, Moulaert VR, van Heugten C, Verbunt JA, Bekkers SC, Wade DT. Life after survival: long-term daily functioning and quality of life after an out-of-hospital cardiac arrest. Resuscitation. 2009;80:517– 522.
https://www.quartztransmuraal.nl/QuartzSite/Protocollen/Regio%20Helmond/Folder%20DNR%20def.pdf
Images are from Anatomography maintained by Life Science Databases(LSDB)
